Disease Education
Disease Education
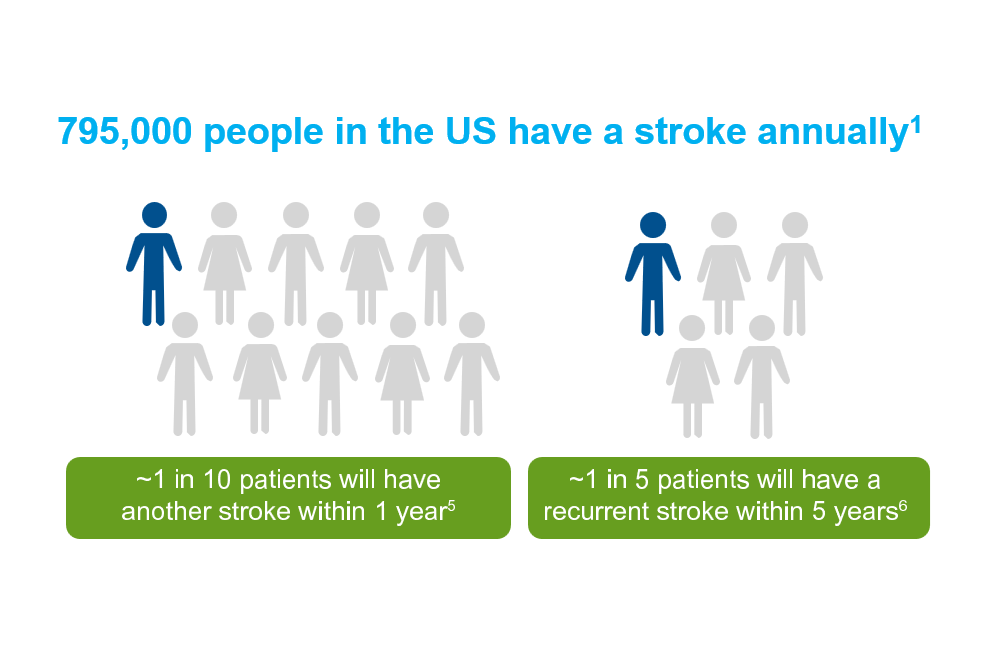
More than 795,000 strokes occur yearly in the US; of those, nearly one-fourth are recurrent strokes1
Despite standard of care, Approximately 1 in 5 patients will have a recurrent stroke within 5 years2
Risk of death and disability is greater in patients with a recurrent stroke3,4
Approximately 1 in 10 patients will have a recurrent stroke within 1 year5
References:
- Kleindorfer DO, et al. Stroke. 2021;52(7):e364-e467.
- Stahmeyer JT, et al. Dtsch Arztebl Int. 2019;116(42):711-717.
- Skajaa N, et al. Neurology. 2022;98(4):e329-e342.
- Chaturvedi S. NEJM Journal Watch Neurology. Dec 21, 2021; https://www.jwatch.org/na54449/2021/12/21/stroke-recurrence-and-long-term-mortality
- Flach C, et al. Stroke. 51(8). 2020;51(8):2435-2444.
- According to the AHA/ASA, a stroke is defined as “an acute episode of focal neurological dysfunction that persists for more than 24 hours”1
- Ischemic stroke is categorized into further subtypes, as seen in the figure here2
- A transient ischemic attack is a period of neurological dysfunction typically lasting under an hour, secondary to cerebral ischemia3
- Characterized by the rapid, progressive loss of neurons, synapses, and myelinated fibers in the brain, the phrase “time is brain” is often used to describe the need for rapid treatment of stroke4,5
- When left untreated, patients can develop long-term complications, including cognitive deficits6
AHA, American Heart Association; ASA, American Stroke Association.
References:
- Tadi P, et al. Acute Stroke. In: StatPearls [Internet]. StatPearls Publishing; 2024.
- Ischemic Stroke (Clots). ASA; 2025; https://www.stroke.org/en/about-stroke/types-of-stroke/ischemic-stroke-clots
- Panuganti KK, et al. Transient Ischemic Attack. In: StatPearls [Internet]. StatPearls Publishing; 2024.
- Saver JL. Stroke. 2006;37(1):263-266.
- Whiteley WN, et al. Stroke. 2014;45(12):3612-3617.
- Gaddipati P, et al. JEMS. 2024; https://www.jems.com/training/building-stroke-ready-communities-the-importance-of-bystander-stroke-education/
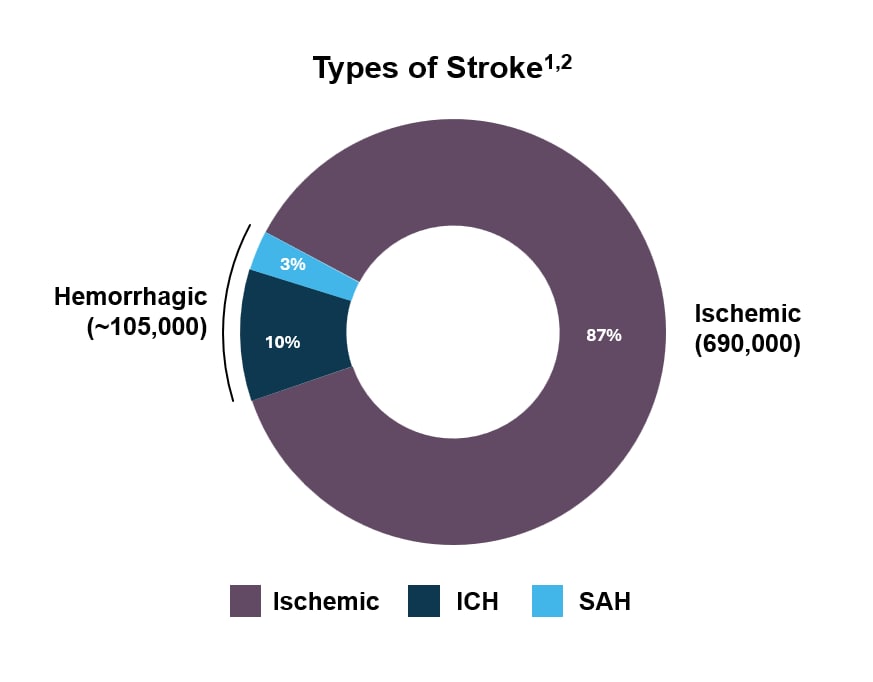
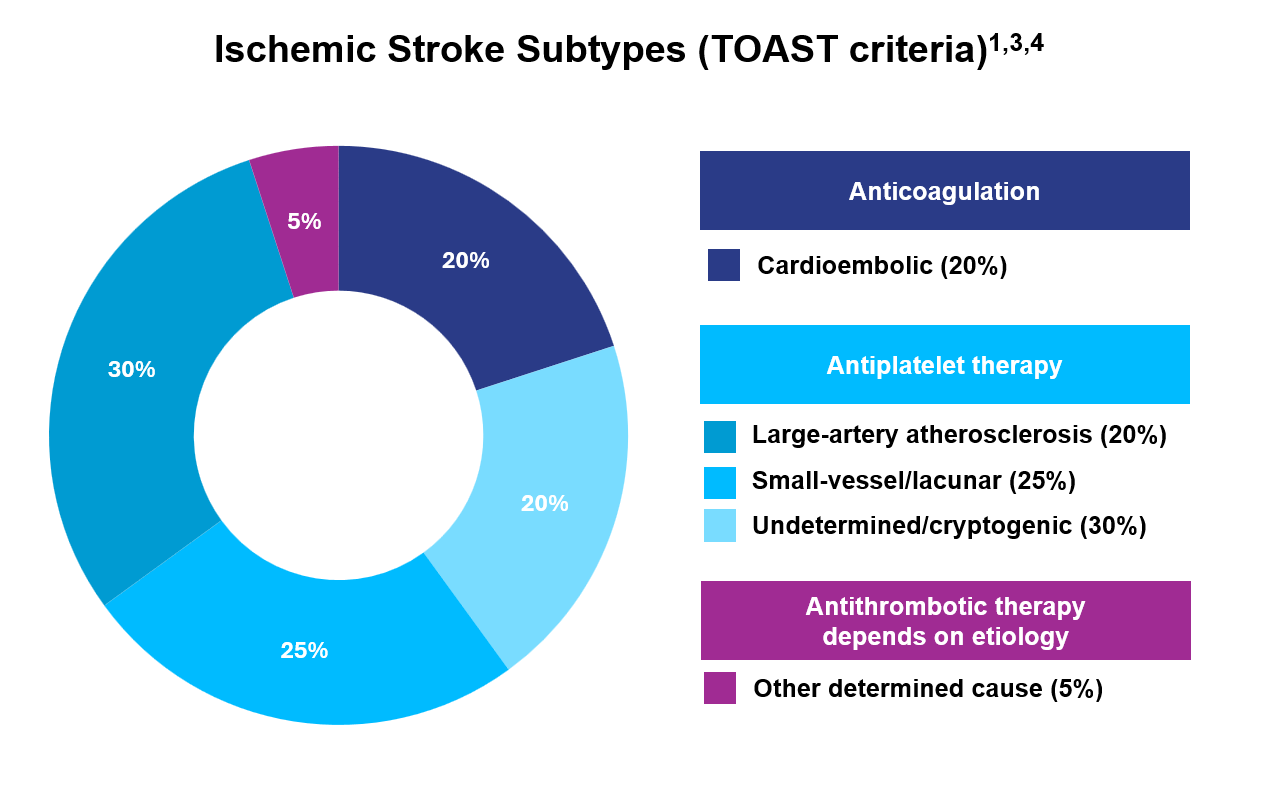
ICH, intracerebral haemorrhage; OAC, oral anticoagulant; SAH, subarachnoid hemorrhage; TOAST, trial of ORG 10172 in Acute Stroke Treatment.
References:
- Kleindorfer DO, et al. Stroke. 2021;52(7):e364-e467.
- Martin SS, et al. Circulation. 2024;149(8):e347-e913.
- Goldemund D. Toast classification of stroke. Stroke Manual: Treatment and Prevention. Accessed September 23, 2024. https://www.stroke-manual.com/toast-stroke-classification/
- Greco A, et al. J Am Col Cardiol. 2023;82(15):1538-1557.
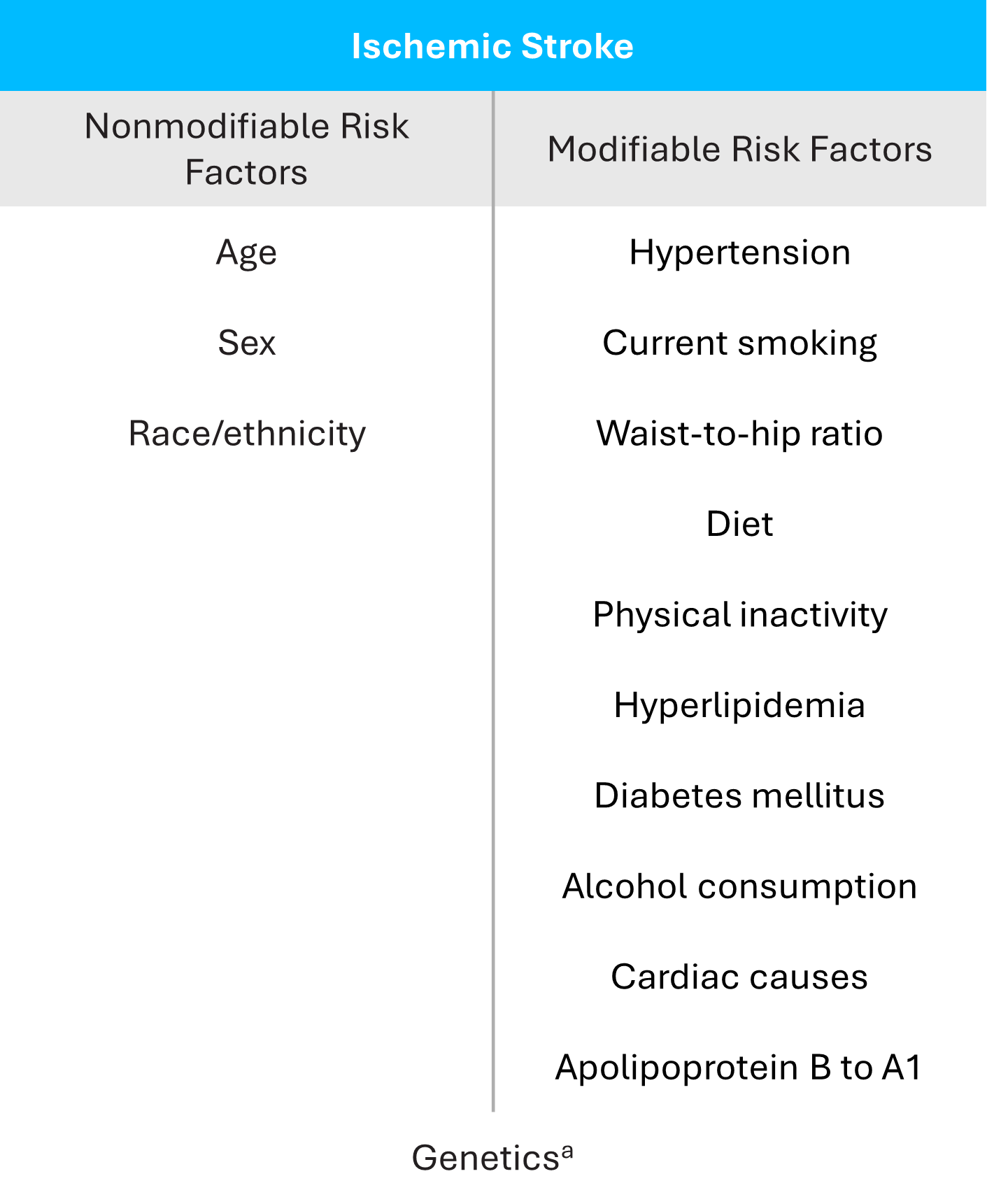
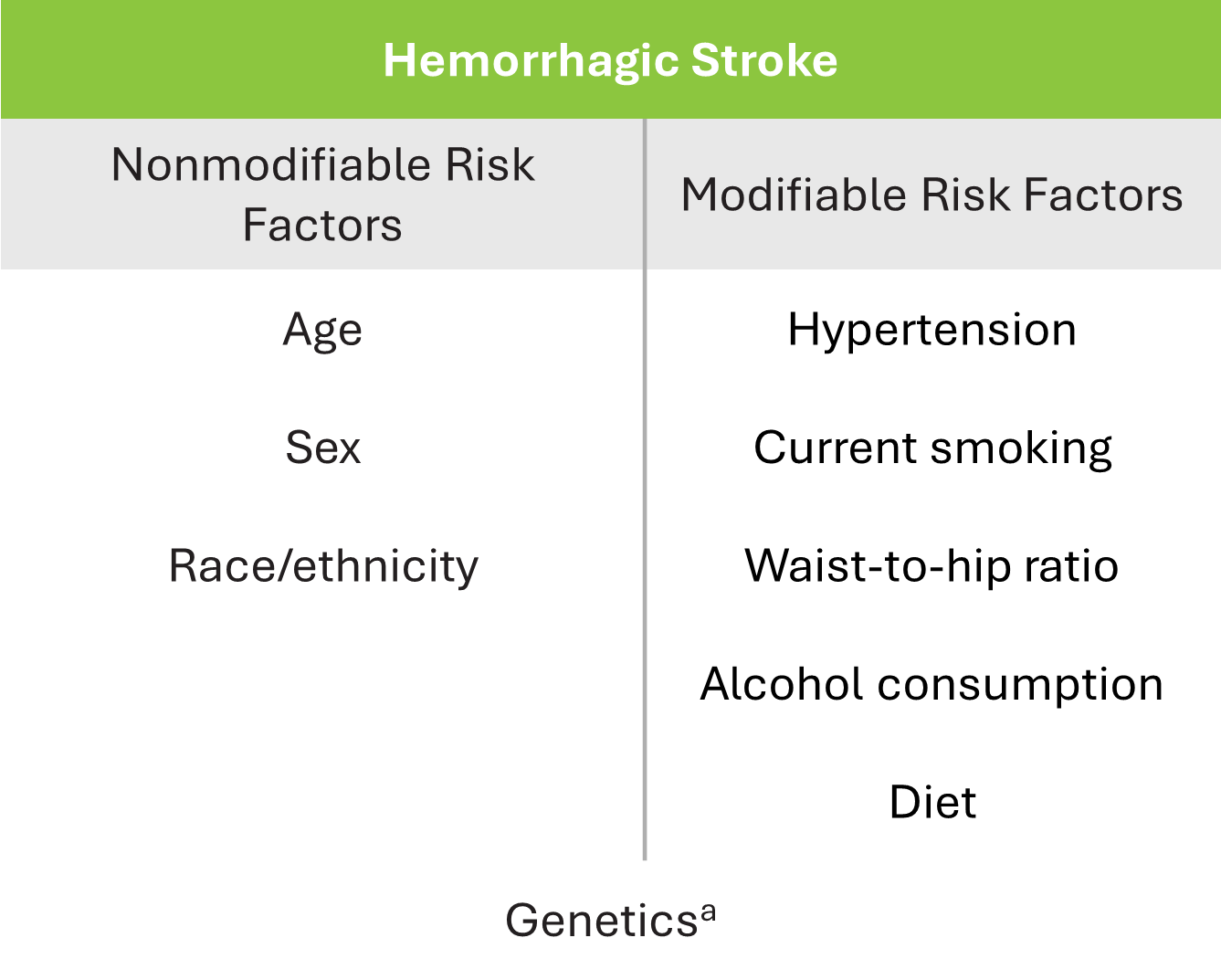
aGenetics is placed in an overlapping location between modifiable and nonmodifiable to represent the fact that genetic risk factors are increasingly recognized as potentially modifiable, either directly or through modification of gene-environment interactions.
Boehme AK, et al. Circ Res. 2017;120(3):472-495.
The Risk of Recurrent Stroke Remains High, Despite Guideline Directed Medical Therapy
The stroke recurrence rate for patients with non-cardioembolic stroke can be >7% in the 3 months following a strokea
The AHA/ASA guidelines recommend switching to SAPT within 90 days because of an increased risk of bleeding with prolonged DAPT in recent minor stroke or high-risk TIA.2 However, the residual risk of recurrent stroke remains for patients with prior ischemic stroke3,4
aData from a randomized, double-blind clinical trial conducted at 114 clinical centers in China of patients randomized to receive aspirin alone (n=2586) or clopidogrel and aspirin (n=2584).
AHA, American Heart Association; ASA, American Stroke Association; DAPT, dual antiplatelet therapy; SAPT, single antiplatelet therapy; TIA, transient ischemic attack.
References:
- Wang Y, et al. N Engl J Med. 2013;369:11-19.
- Kleindorfer DO, et al. Stroke. 2021;52:e364–e467.
- Diener HC, et al. Lancet. 2004;364(9431):331-337.
- SPS3 Investigators. N Engl J Med. 2012;367:817-825.
- Leifheit EC, et al. Stroke. 2022;53(11):3338-3347.
- Stahmeyer JT, et al. Dtsch Arztebl Int. 2019;116(42):711-717.
Increased Risk of Death With Recurrent Stroke
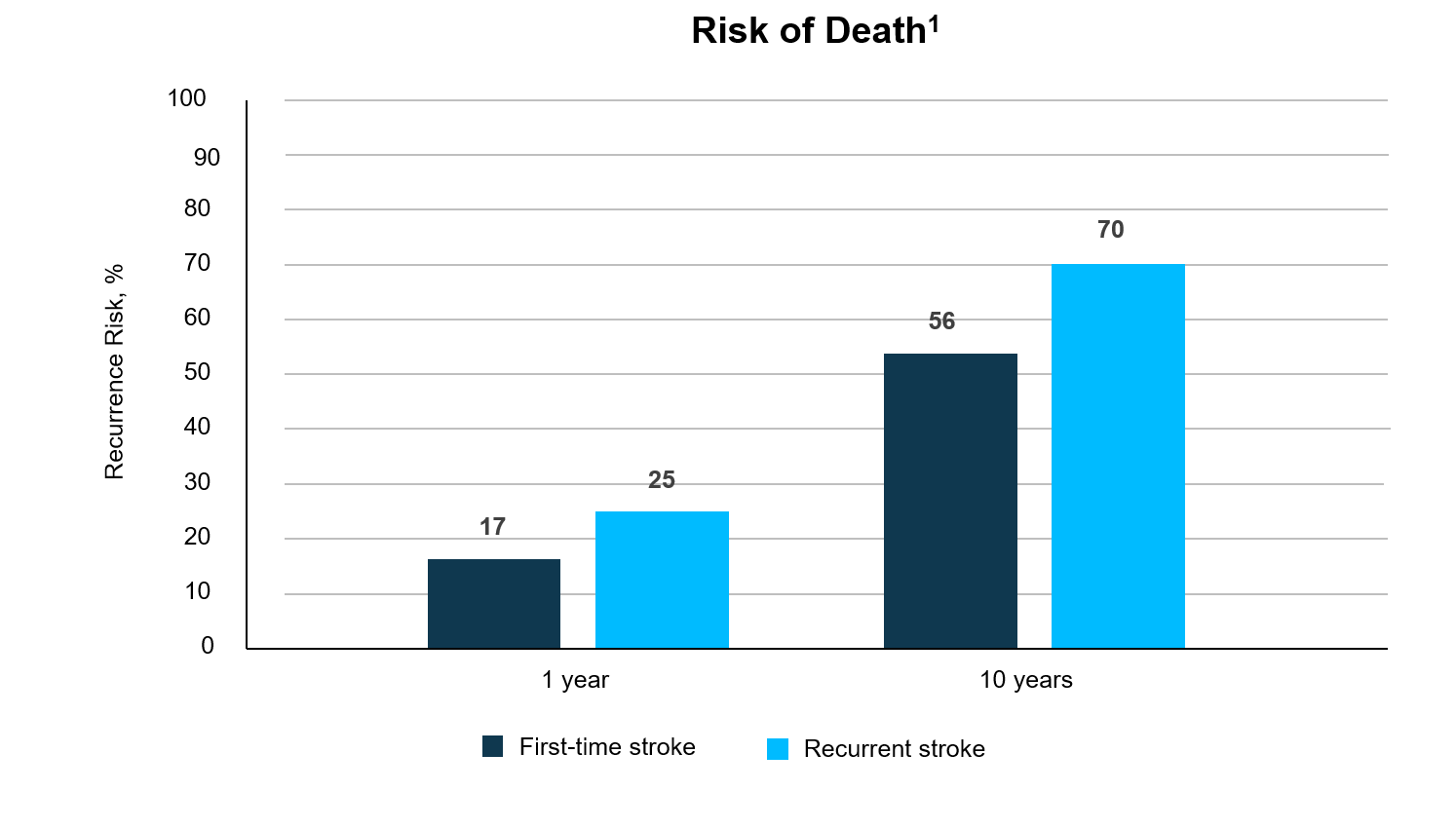
One study found that the risk of death at 30 days after first recurrent stroke was 41%, while the risk after first-ever stroke was 22%2
Risk of death is greater for patients with a recurrent stroke vs patients with a first-time stroke1,2
References:
- Skajaa N, et al. Neurology. 2022;98(4):e329-342.
- Hardie K, et al. Stroke. 2004;35(3):731-735.
Residual Risk of Recurrent Stroke in Contemporary Studies
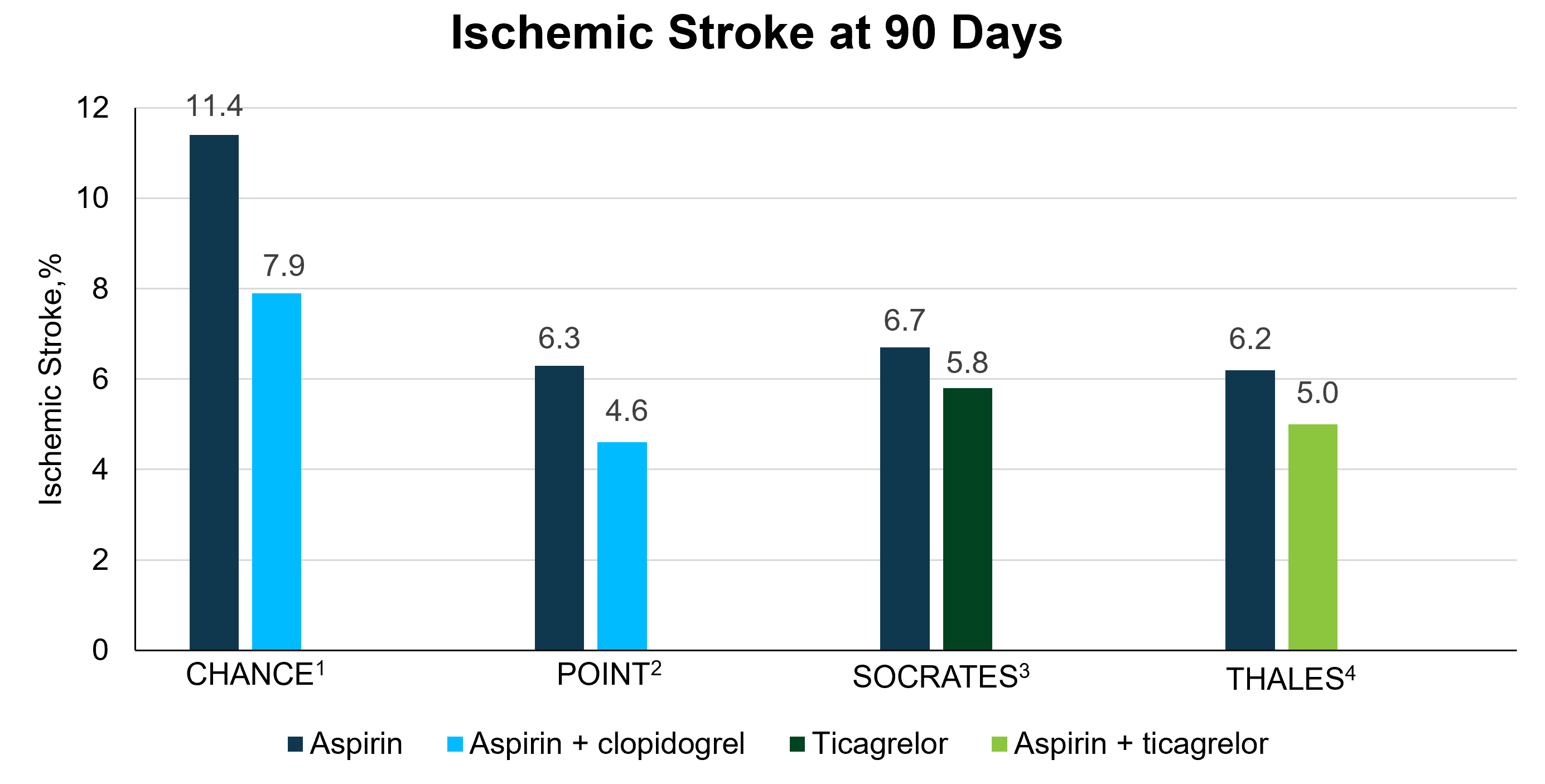
CHANCE, Clopidogrel in High-Risk Patients with Acute Nondisabling Cerebrovascular Events; POINT, Platelet-Oriented Inhibition in New TIA and Minor Ischemic Stroke; SOCRATES, Acute Stroke or Transient Ischemic Attack Treated with Aspirin or Ticagrelor and Patient Outcomes; THALES, Acute Stroke or Transient Ischemic Attack Treated With Ticagrelor and ASA for Prevention of Stroke and Death.
References:
- Wang Y, et al. N Engl J Med. 2013;369(1):11-19.
- Johnston SC, et al. N Engl J Med. 2018;379(3):215–225.
- Johnston SC, et al. N Engl J Med. 2016;375(1):35-43.
- Johnston SC, et al. N Engl J Med. 2020;383(3):207-217.
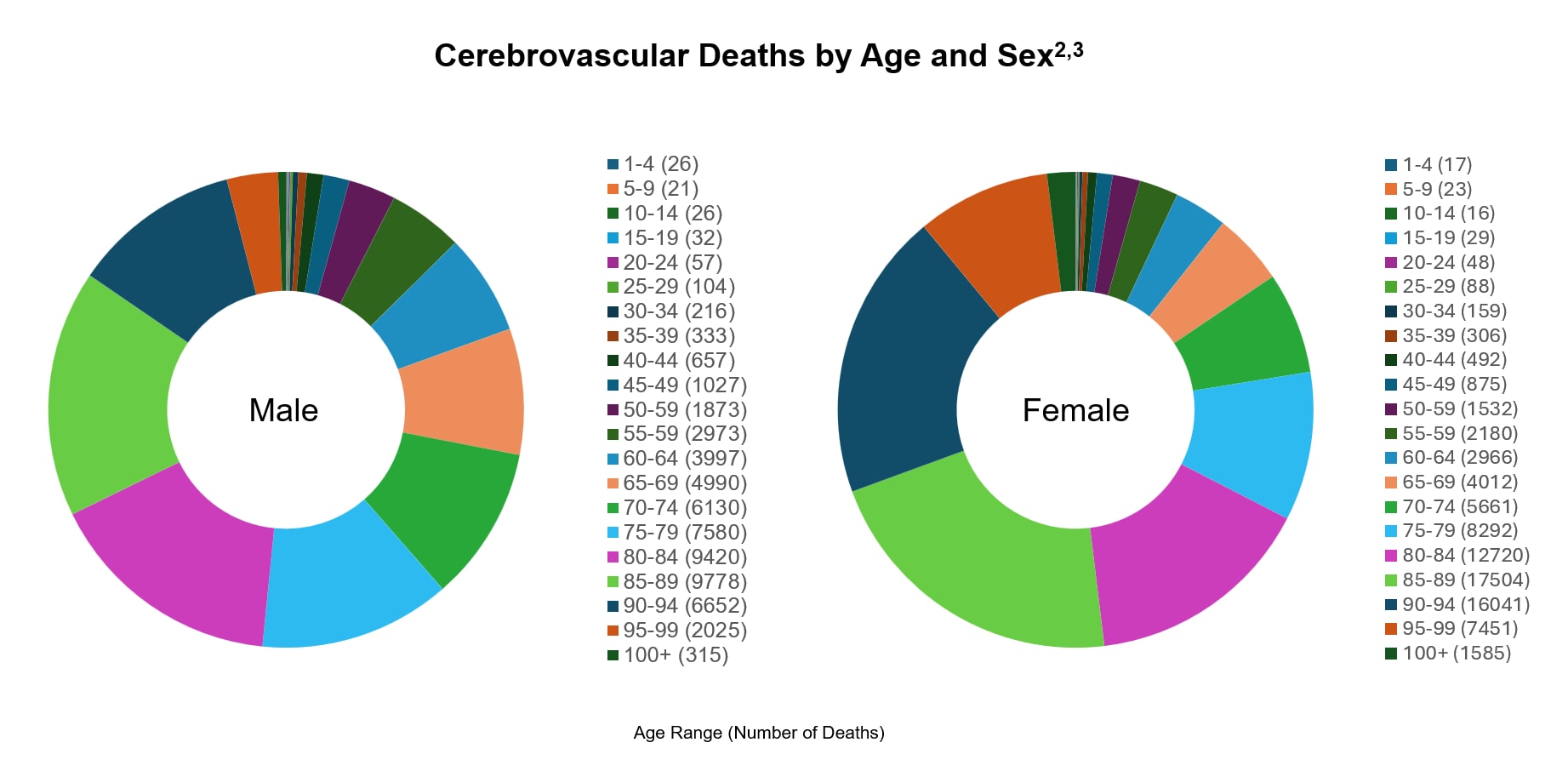
In 2019, stroke ranked as the third leading cause of death among women in the United States, compared to fifth among men. Women represented 57.1% of all stroke-related deaths that year. Stroke accounted for 6.2% of total female deaths and 4.4% of total male deaths. Overall, women experienced about 55,000 more fatal strokes annually than men.²
In 2019, stroke ranked as the third leading cause of death among women in the United States, compared to fifth among men.
Women represented 57.1% of all stroke-related deaths that year. Stroke accounted for 6.2% of total female deaths and 4.4% of total male deaths. Overall, women experienced about 55,000 more fatal strokes annually than men.2
References:
- Age-adjusted stroke mortality rates in stroke. American Heart Association; 2024. www.heart.org
- Rexrode KM, et al. Circ Res. 2022;130(4):512-528.


